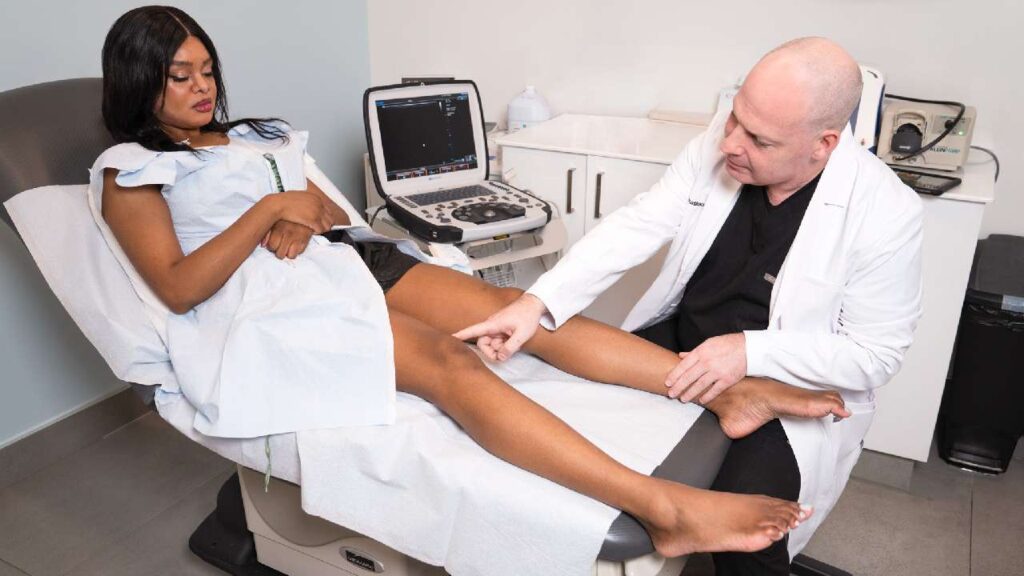
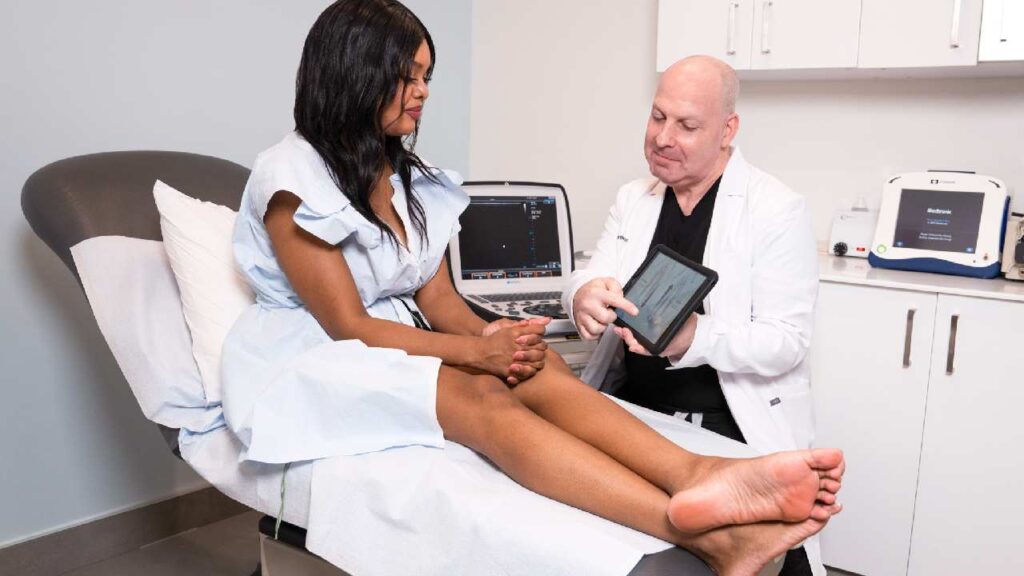
Myth or Fact: Varicose Veins and Spider Veins Are the Same
Some people assume varicose veins and spider veins are the same issue. While they share certain causes, they are two different types of vein damage. Varicose veins are swollen, bulging, twisted veins that result from excess pressure inside the vein. The most common reason for pressure elevation is a faulty valve in a deeper vein. This allows blood to leak backward through the vein and accumulate, which engorges and contorts the veins at the surface, making them varicose.
A spider vein can result from the same impetus, but it can also be caused by external pressure, including a skin injury, sun damage, squeezing a pimple, or extreme temperatures. These triggers for spider veins are more common in areas with thin skin, like the face, while internal pressure more commonly causes spider veins in the legs. Spider veins have a different appearance from varicose veins. They are thin, spindly, and non-protuberant. They often form in clusters with a central point of origin and branches of blood vessels radiating outward. They’re called telangiectasias, and they can resemble a spider or a spider’s web, hence the nickname. But in some patients, spider veins look more like a bruise.
Book an appointment with a vein doctor who treats both kinds of vein damage since having one type increases the odds that you’ll develop the other. If you have either spider or varicose veins in your legs, you might also have a common issue called Chronic Venous Insufficiency. Treating this is essential to preventing more vein damage, as you’ll learn about later in this article.
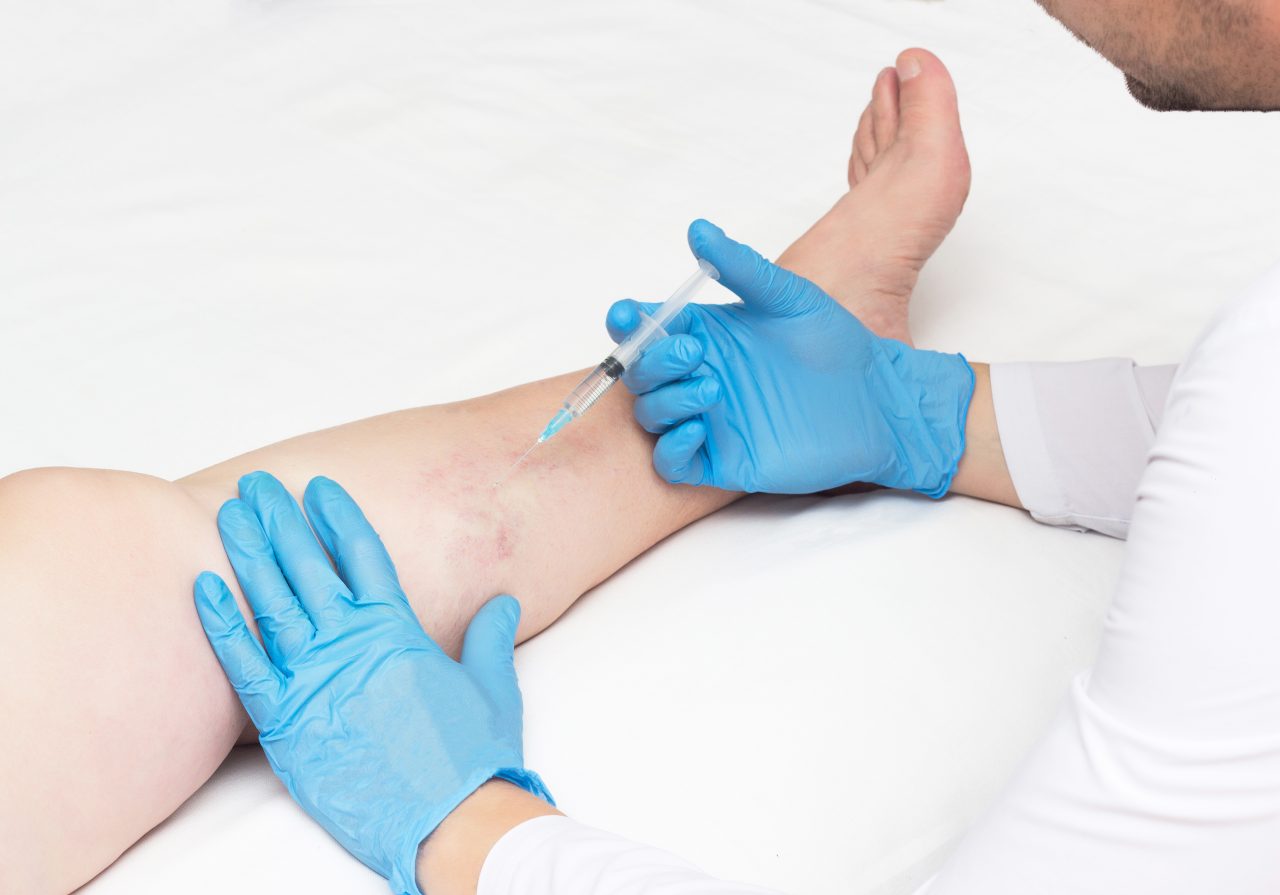
Myth or Fact: Family History Is the Top Predictor of Veins
Family history is the top predictor of developing varicose veins or spider veins. If a close relative has them, it increases your risk by up to 50 percent. If both of your parents have them, you have a greater than 90 percent chance of developing them. There are other risk factors as well. Obesity, hormone fluctuations, sedentary lifestyles, gender, and aging all play a role. If these bothersome blood vessels run in your family, see a vein specialist early to minimize your risk.
Myth or Fact: Crossing Your Legs Causes Varicose Veins
Crossing your legs does not cause varicose veins. As mentioned above, internal pressure is the main cause of varicosities. Valve failure and Chronic Venous Insufficiency are often the problem that creates internal venous pressure. However, if you have varicose veins, crossing your legs for an extended period of time can exacerbate symptoms, including swelling and cramping in the legs. Sitting or standing for long periods of time can also exacerbate the uncomfortable symptoms of varicose veins. Many patients experience heaviness, itching, restlessness, pain, and fatigue in their legs, especially at the end of the day. If this applies to you, take breaks to move around throughout the day, and elevate your legs above heart level while relaxing at night. Visit a vein specialist to eliminate both the visible damage and the unpleasant symptoms.
Myth or Fact: Only Women Develop Varicose Veins
Varicose veins are more common in women because pregnancy, birth control usage, menopause, and hormone replacement therapy affect blood pressure and vein walls. However, as people age, the statistics become more similar between men and women. Around 25 percent of women and 15 percent of men will develop vein damage in their lifetime. After age 50, 55 percent of the cases are in women, and 45 percent are in men. So, while women are more prone to them, it’s a myth that men don’t develop varicose veins. If you have bulging, twisted veins, don’t assume it’s from exercise or strenuous activity. It might be a varicose vein.
Myth or Fact: Aging Doesn’t Cause Varicose Veins
Even the healthiest individuals can develop varicose veins as they age because aging weakens vein walls. As blood vessels lose elasticity, it becomes harder for valves in the veins to close tightly. This lets blood flow in reverse and build pressure in the vein. Maintain a healthy weight and active lifestyle if you’re able to, but don’t despair if you develop one of these unsightly blood vessels anyway. Over 40 million Americans have them, and treatment is quick and easy.
Myth or Fact: Vein Stripping is a Top Varicose Vein Treatment
Vein stripping surgery was once a common solution for varicose veins, but it’s now a last resort. Minimally invasive technology has largely replaced surgical vein extraction. Vein doctors can now close veins inside the body with tiny tools rather than cutting them out. If you’ve delayed a vein consultation because you don’t want surgery, don’t delay any longer. The sooner you seek treatment, the less likely it is that you’ll need to have vein stripping done.
Myth or Fact: Compression Stockings Treat Twisted Veins
Compression stockings don’t remove twisted veins. The only way to fully eliminate a damaged vein is to close it off or cut it out and reroute blood into healthier veins nearby. For some patients, compression therapy can reduce symptoms including cramping and swelling. But for other patients, compression is ineffective or even dangerous. Don’t try these stockings without a doctor’s approval. If you’re a candidate for compression, our vein specialists will select the right size, so you don’t endure insufficient or excessive pressure.
Myth or Fact: Every Vein Specialist Offers the Same Methods
No two vein clinics offer the same procedures. Some clinics are run by board certified vein doctors, while others are run by estheticians or other practitioners who didn’t study vein medicine or vascular surgery. If you want exceptional care, cutting-edge treatments, and insurance coverage, always choose a board certified vein doctor. This will ensure your treatment is safe, successful, and permanent, unlike the methods used at most cosmetic treatments. The top New York vein doctors include Dr. Juan Montoya, Dr. Sareh Rajaee, and Dr. Shane Volney.
Myth or Fact: Treating Vein Damage Is Optional
It’s true that some veins don’t become symptomatic. But it’s also true that many people have mild, moderate, and even life-threatening complications from unhealthy veins. It’s impossible to predict how your veins will progress, and your symptoms aren’t always a valid indication of what’s happening in deeper blood vessels. If you want to avoid leg cramping, swelling, restlessness, heaviness, fatigue, and pain, as well as venous ulcerations, venous stasis dermatitis, blood clots, profuse bleeding, and hyperpigmentation, consult a vein doctor. Our innovative vein specialists can spot trouble in deeper veins before it manifests at the surface. We look forward to protecting your vascular health with our gentle vein treatments.