How Do You Treat an Occlusive Blood Clot in a Deep Vein?
A deep vein thrombosis (DVT) is a blood clot in a deep vein. They often develop in the legs, and occasionally in the arms or abdomen. A deep vein thrombosis can quickly turn serious because it can travel to the lungs. This can cause a pulmonary embolism, wherein one or more arteries in the lungs are blocked by the DVT. When a DVT causes a pulmonary embolism, it’s called venous thromboembolism. This is often fatal.
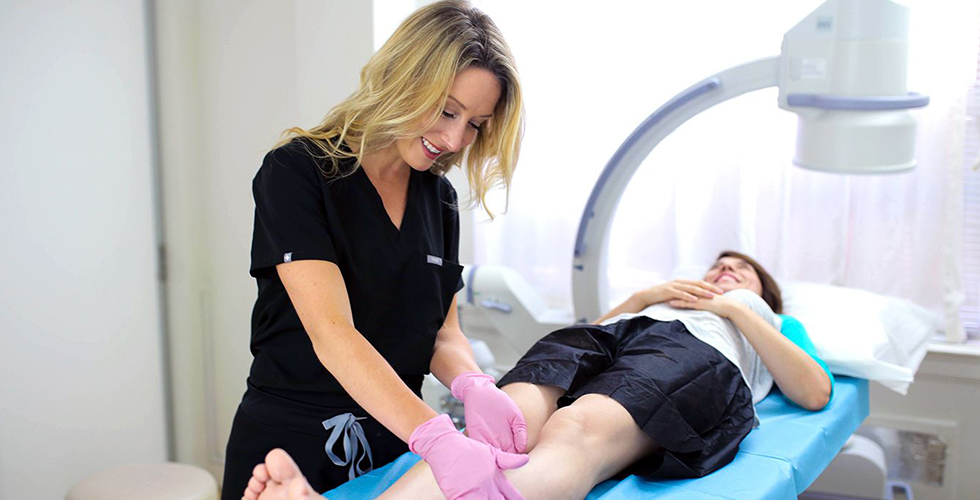
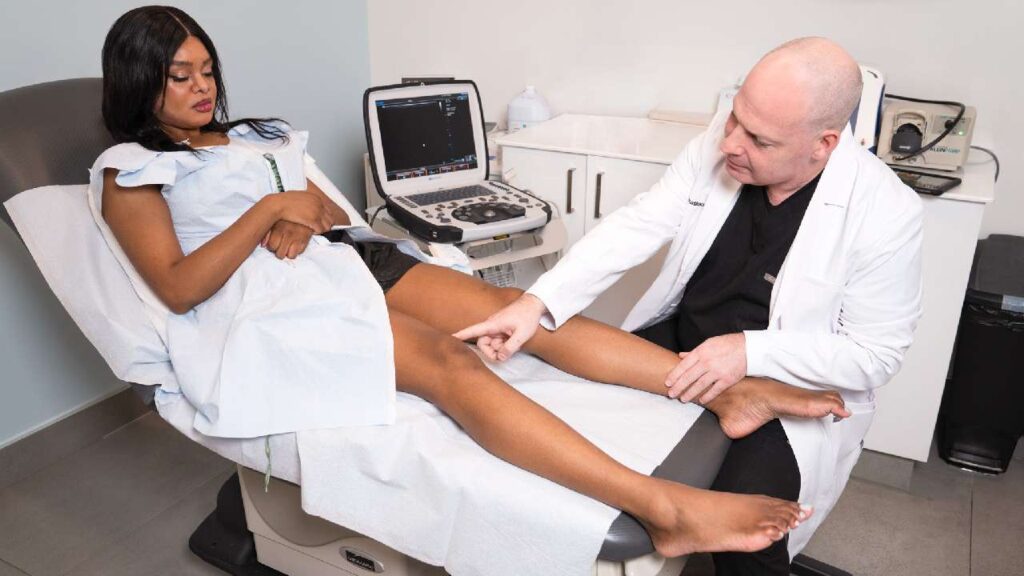
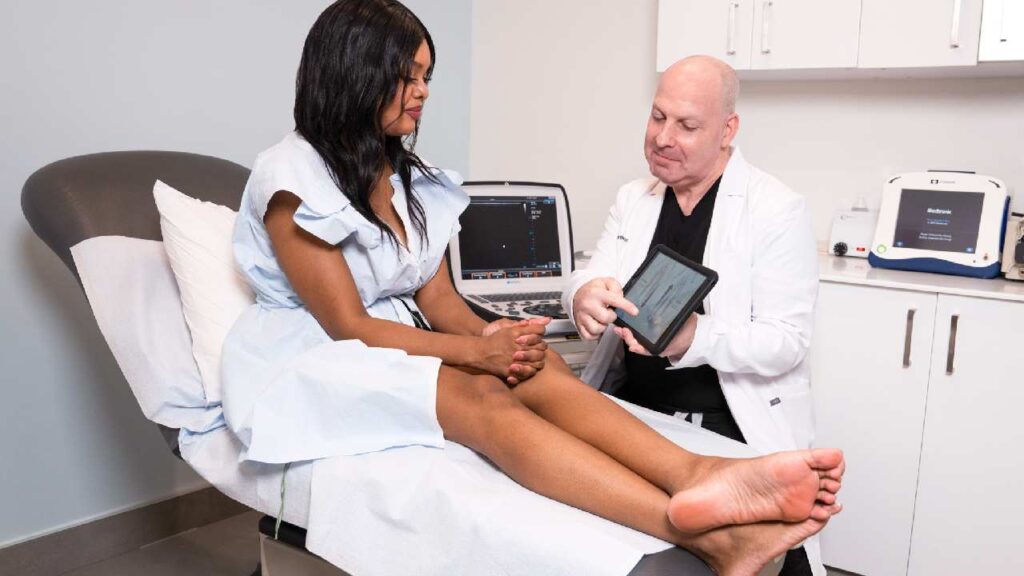
Deep vein thrombosis treatment requires great expertise to prevent the clot from breaking loose and impacting your lung. Book an appointment with Harvard-trained vein doctors in New York to ensure safe treatment. DVT treatment should always start with a physical examination, followed by a blood test or Duplex Ultrasound scans that locate the clot and determine the best course of action. The best treatment depends on several variables that are unique to you. Here are some of the top options.
- Blood Thinners: If the clot is small, vein doctors might prescribe anticoagulants. These help prevent blood clots from getting bigger and also help stop new ones from forming. Blood thinners are administered in pill form or through an IV. These carry risks, so your doctor will determine the best one for you. When blood is thinned, you bleed easier, and it’s easier for the clot to travel. So, these aren’t always advised for large clots that could occlude an artery. Nor are they advised for pregnant patients or patients with certain diseases. If you take a blood thinner, see your vein doctor regularly to monitor the size and location of the clot.
- Thrombolytics: For larger clots that don’t respond to other medicines, thrombolytic clot busters can be used. They’re delivered through an IV or a catheter that’s inserted in the affected vein. They can cause significant bleeding, so they’re reserved for large, serious clots.
- Vena Cava Filters: If something prohibits you from taking medicines, vein doctors can place a filter in your inferior vena cava, which is an abdominal vein that transports blood from the lower body to the heart. These filters are like small metal baskets that trap blood clots, so a DVT can’t travel to your lungs.
- Compression Stockings: Some patients can wear compression stockings to help the clot dissolve or pass through. These must be sized by your vein doctor since too much compression is dangerous and too little pressure is ineffective. A vein doctor should analyze your vasculature before deciding on this method, so don’t try these without seeing a vein specialist first.
Is Posterior Tibial Vein Thrombosis Treatment Required?
The posterior tibial vein in the calf is a common location for a blood clot in leg veins. Vein doctors will assess your symptoms, bleeding risk, mobility, blood clot history, and how close the clot is to proximal veins before selecting treatment. Some posterior tibial vein clots can be monitored if the patient can increase leg exercises and use medication or compression. Others might need immediate treatment, which is often an anticoagulant or filter.
Are the Superficial Venous Thrombosis Guidelines Different?
Blood clots can also develop in surface veins. These aren’t as life-threatening as DVTs, because they don’t travel to the lungs. But superficial blood clots produce other complications. These include profuse bleeding, hyperpigmentation, ulcerations, venous stasis dermatitis, pain, and swelling, as well as the development of varicose veins and spider veins. Here’s how vein doctors treat superficial vein thrombosis.
- Vein Treatment: Blood clots often elevate pressure in the vein, which can cause swollen varicose veins or spider veins that branch out from the pressurized vein. For many patients, treating a deep blood clot also involves treating damaged veins at the surface. Always select a board certified vein doctor for this, not a cosmetic or dermatological clinic.
- Compression Stockings: If a patient doesn’t need vein treatment, compression stockings might be advised. As mentioned, these require a vein doctor’s guidance to ensure optimal compression. These can help prevent new clots from forming as well, so ask your vein specialist if they’re right for you.
- Non-Steroidal Anti-Inflammatory Medication: Medicines like ibuprofen can decrease inflammation in veins and improve circulation. However, don’t try these without asking your doctor. They’re not safe for all clots, and they can cause internal bleeding. NSAID therapy can irritate the stomach lining and cause GI bleeding.
Is the Best Phlebitis Treatment Hot or Cold Therapy?
Phlebitis is inflammation of a vein with or without blood clots. A clot is often involved, but sometimes phlebitis results from vein wall damage after an injury or surgery. The symptoms include pain, redness, and warmth, which are also blood clot symptoms. Visit a vein doctor to rule out a superficial or deep vein thrombosis.
If you only have phlebitis, it should resolve with self-care. Your vein doctor might suggest compression stockings, anti-inflammatory medication, or blood thinners. Warm water compresses are advised for many patients with phlebitis. Your doctor might advise you to elevate your legs while at rest and avoid long periods of sitting or standing still if you’re able to move around.
Can Dr. Morse Upper Circulation Tinctures Treat Blood Clots?
Some patients inquire about supplements like Dr. Morse circulation tinctures. These have no clinical studies on safety or efficacy. They’re not regulated by the FDA or advised for blood clots. Furthermore, some patients shouldn’t thin their blood, depending on the size and location of the clot and coexisting medical conditions.
Ask a board certified vein doctor before trying anything for circulation. This includes caffeine and anti-inflammatories. If you’re unable to take medications for veins, our doctors have several gentle methods for restoring circulation.
What Helps Prevent Blood Clots from Forming?
Blood clots aren’t always preventable, but you can lower your risk of developing them. Visit a vein specialist before attempting anything new. Here’s what we often suggest.
- Maintain a healthy weight: Excess weight burdens your veins, increasing the incidence of blood clots.
- Exercise daily: Muscle contractions pump blood out of veins. The more you move, the less likely it is for blood to clot in your veins. If you can’t stand, try seated calf raises or ankle rotations.
- Elevate your legs while at rest: When you’re lying down, prop your legs above heart level so blood flows away from your feet. Leg veins are prone to blood pooling that contributes to blood clots.
- Stop smoking: There are countless reasons to do this. Your cardiovascular health is a primary reason. Smoking weakens your lungs and heart. A DVT that travels to a compromised lung is often fatal.
- Moderate sodium and caffeine: You might need to cut sodium and caffeine out or reduce them. These elevate blood pressure, so ask your doctor if they’re safe for you, especially if you’ve had blood clots before.
- Examine veins during pregnancy, birth control use, menopause, and HRT: Hormone fluctuations stretch blood vessels and increase blood volume. If you develop spider veins or varicose veins during hormonal changes, see a vein doctor. If you develop symptoms of DVT, like sudden redness, warmth, or, swelling, go to the hospital.
Can I Wear Compression Stockings to Prevent Blood Clots?
Compression stockings are advised for some patients, but not everyone. Compression therapy can be dangerous for patients with certain clots and compromised cardiovascular health. Don’t purchase them without a vein consultation. The size and type determine safety and efficacy.
Where is the Best DVT Treatment Near Me?
To treat DVT safely and effectively, visit any of our award-winning New York vein clinics. Our Ivy League vein specialists are renowned for vascular care with minimally invasive methods. Our vein clinics are located in Midtown, the Financial District, and Hartsdale, New York.